Every year, millions of people in the U.S. stop taking their medicine-not because it doesn’t work, but because they don’t understand what they’re taking. This isn’t about forgetting pills or side effects. It’s about generic medications. Many patients switch from a brand-name drug to a generic version, only to panic when the pill looks different, the price drops, or a pharmacist says, "It’s the same thing." The result? They quit. And that’s not just a personal mistake-it’s a public health crisis.
What Exactly Is a Generic Medication?
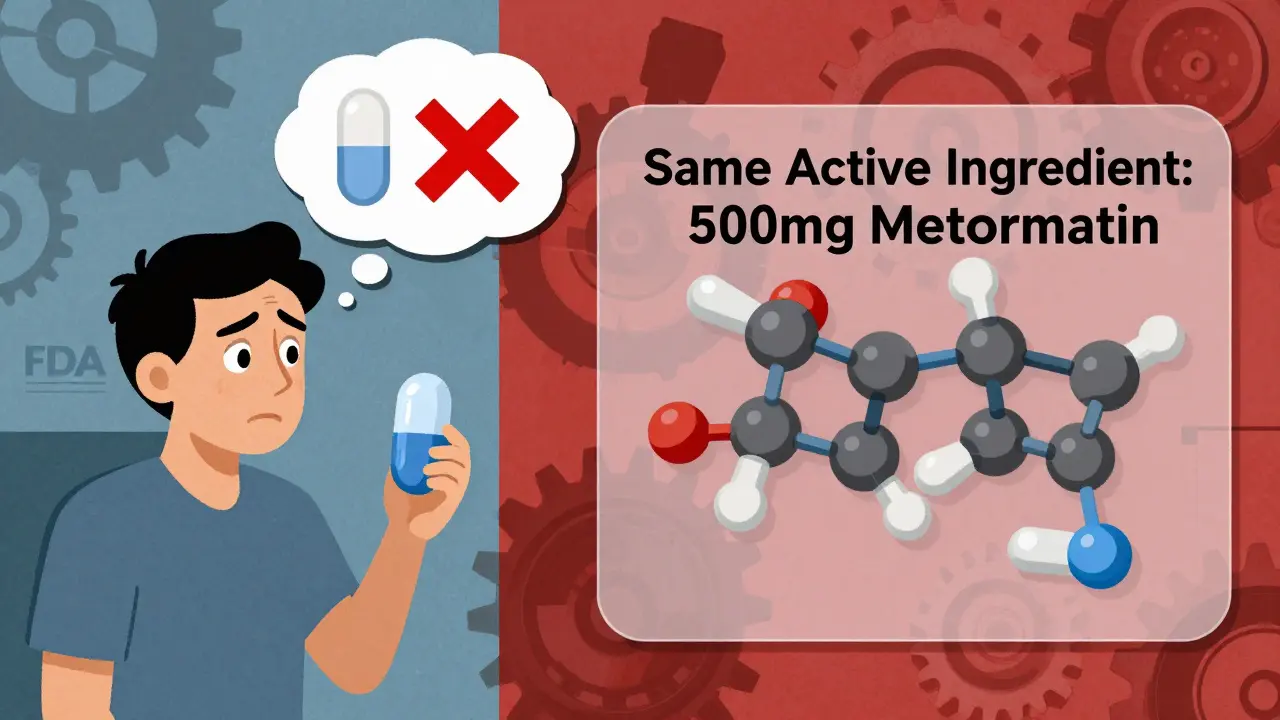
A generic drug is not a copycat. It’s not a cheaper imitation. It’s the exact same medicine as the brand-name version, just without the marketing budget. The FDA requires generics to contain the same active ingredient, in the same strength, and in the same way as the original. That means if you’re taking metformin for diabetes, whether it’s called Glucophage or just "metformin," your blood sugar is being controlled by the same molecule. The difference? Inactive ingredients. Things like dyes, fillers, or coatings that change the pill’s color, shape, or how fast it dissolves. These don’t affect how the drug works-but they sure mess with your head.
Here’s the kicker: 68% of patients believe generic drugs are less effective than brand-name ones. Meanwhile, studies show that 47% of people with low health literacy don’t realize generics have the same active ingredient. That’s not fear-it’s ignorance. And ignorance costs lives.
Why Health Literacy Matters More Than You Think
Health literacy isn’t about being smart. It’s about being able to read a prescription label, understand a pharmacist’s instructions, or know what "80-125% bioequivalence" really means (spoiler: it means the drug works just as well). The CDC says only 12% of U.S. adults have proficient health literacy. That means nearly nine out of ten people struggle with basic medical info.
For generics, this gap is deadly. A person with low health literacy is:
- 32% more likely to be hospitalized because of a medication mistake
- 2.5 times more likely to take the wrong dose
- 23% less likely to stick with their treatment plan
And here’s the worst part: when someone stops taking a generic because they think it’s "not the real thing," they’re not just risking their health-they’re costing the system money. The U.S. spends $1.2 billion a year on unnecessary brand-name prescriptions because patients don’t understand generics. That’s money that could go to more care, better research, or lower premiums.
Who Gets Left Behind?
This isn’t a problem that affects everyone equally. Immigrants who speak limited English, older adults who can’t read small print, people with low incomes, and those with mental health conditions are hit hardest. A 2025 study found that non-English speakers are 3.2 times more likely to misunderstand generic medication labels than native speakers. Why? Because most instructions are written in medical jargon, printed in tiny fonts, and rarely translated.
One patient on Reddit shared: "I stopped my blood pressure pill because the generic was blue. The brand was white. I thought they switched me to something else." That’s not paranoia. That’s a system failure. The pill’s color changed because the manufacturer used a different dye. The drug? Identical. But without clear communication, trust breaks down.

How Pharmacists Are Trying to Fix This
Pharmacists are on the front lines. They spend an average of 4.2 minutes explaining generics to patients. But if the patient has low health literacy? That jumps to nearly 10 minutes. That’s not sustainable. And even then, many pharmacists use the same old script: "It’s the same drug." That’s not enough.
What works? The Teach-Back method. Instead of telling patients what generics are, pharmacists ask them to explain it back. "Can you tell me in your own words why this blue pill works the same as the white one?" If they can, they understand. If not, the conversation continues. Studies show this simple trick cuts misunderstandings by 42%.
Visual aids help too. Showing side-by-side pictures of brand and generic pills with labels like "Same active ingredient: 500mg metformin" makes the difference obvious. Some clinics now use pill apps that scan a pill and show its name, purpose, and whether it’s generic. One 2022 study found patients using these apps recognized generic drugs 35% better than those who just got verbal instructions.
The Real Cost of Not Understanding
When patients stop taking their meds because they think generics don’t work, they end up in the ER. Or worse-they end up in a hospital bed from a preventable stroke, heart attack, or diabetic complication. The average cost of one preventable hospitalization due to a medication misunderstanding? Over $15,000.
And here’s the irony: generics make up 90% of all prescriptions filled in the U.S. But they only cost 23% of total prescription spending. That’s because they’re cheap-and effective. If everyone understood that, the U.S. could save $675 per person annually just by reducing ER visits and hospital stays tied to medication confusion.
Yet only 38% of healthcare organizations have any program to teach patients about generics. That’s not a lack of resources. It’s a lack of priority.

What’s Changing Now?
There’s hope. In January 2023, the FDA launched the "Generics Awareness Campaign," using simple language, videos, and infographics to explain what generics really are. The CDC added "improving understanding of medication alternatives" to its 2023 Health Literacy Action Plan. And starting in 2024, Medicare Part D plans must assess patients’ health literacy before dispensing medications.
Some health systems are testing something even bigger: embedding health literacy checks into electronic records. If a patient’s record shows low literacy, the system automatically flags their prescription and triggers a pharmacist call or printed visual guide. Pilot programs saw a 31% improvement in patient understanding within six months.
And it’s working. Health systems that implemented full medication literacy programs saw generic-related errors drop by 27% in just 18 months. Patients who received clear, simple explanations were 83% more likely to keep taking their meds.
What You Can Do
If you or someone you care about is on a generic medication:
- Ask: "Is this the same as the brand-name drug?" Don’t be shy. Pharmacists expect this question.
- Look at the label. The active ingredient is listed first. If it matches the brand, it’s the same medicine.
- Use a pill identifier app. Many are free and work offline.
- Ask for plain-language materials. Most pharmacies have them-just ask.
- Use the Teach-Back method yourself: "So, you’re saying this blue pill has the same medicine as the white one?" If they say yes, you’ve got it.
And if you’re a caregiver, parent, or community health worker: Don’t assume someone understands. Show them. Explain it twice. Ask them to repeat it. That’s how you save lives.
Are generic medications as safe as brand-name drugs?
Yes. The FDA requires generic drugs to meet the same strict standards as brand-name drugs for quality, strength, purity, and stability. They must contain the same active ingredient, in the same amount, and work the same way in the body. The only differences are in inactive ingredients-like color, shape, or filler-which do not affect how the drug works.
Why do generic pills look different from brand-name ones?
Generic manufacturers can’t use the same color, shape, or logo as the brand-name drug because of trademark laws. That’s why a generic version might be blue instead of white, or oval instead of round. These changes are purely cosmetic and have no effect on the drug’s effectiveness or safety.
Can I trust generics if they’re so much cheaper?
Yes. Generics are cheaper because they don’t need to repeat expensive clinical trials or spend billions on advertising. The active ingredient is identical, and the manufacturing process is closely monitored by the FDA. A generic drug must prove it delivers the same amount of medicine into the bloodstream as the brand-name version-within a very tight range. If it doesn’t, it’s not approved.
What should I do if I think the generic isn’t working?
Don’t stop taking it. Talk to your pharmacist or doctor first. Sometimes, changes in how you feel are due to other factors-like diet, stress, or other medications. Rarely, a patient may react differently to inactive ingredients (like dyes or fillers), which can cause side effects. But this doesn’t mean the drug isn’t working. Your provider can help determine if it’s a true issue or just a perception gap.
How can I check if a pill is generic or brand-name?
Look at the prescription label. The active ingredient (like "lisinopril" or "sertraline") will be listed first. If it matches the name of your original brand, it’s a generic. You can also use free pill identifier apps (like Drugs.com or Medscape) to scan or search the pill’s imprint, color, and shape. These tools show you the exact drug, whether it’s generic or brand.
Why do some doctors still prescribe brand-name drugs?
In most cases, it’s not because the brand is better. It could be because the patient had a bad reaction to a specific generic’s inactive ingredient, or because the generic wasn’t available when the prescription was written. Sometimes, insurance restrictions or prior authorization rules make it easier to prescribe the brand. But for 90% of prescriptions, a generic is not just cheaper-it’s equally effective.






Mariah Carle March 1, 2026
I just stopped my generic blood pressure med because it turned from white to blue 😔 I thought they switched me to something experimental. Turns out? Same damn pill. Why does the system make us feel like we're being scammed? 🤦♀️
Justin Rodriguez March 2, 2026
I work in a community pharmacy. We've started using visual pill cards with side-by-side images of brand vs generic. Patients who see it don't panic. They nod and say, 'Oh. So it's the same.' Simple. Effective. Costs nothing. Why isn't this standard everywhere?
Raman Kapri March 3, 2026
The FDA's standards are not as rigorous as they claim. Generic manufacturers often outsource production to countries with lax regulatory oversight. The bioequivalence range of 80-125% is a joke. Some patients experience clinically significant variations. This is not a literacy issue-it's a systemic failure of oversight.
Megan Nayak March 3, 2026
Let me get this straight. We’re blaming patients for not understanding that a blue pill is the same as a white one? 🤡 The system doesn’t just fail to educate-it actively obscures. Pill color changes because of trademark laws? That’s not a coincidence. That’s corporate theater. And now we’re asking people to trust a system that deliberately confuses them? I’m not shocked. I’m disgusted.
Tildi Fletes March 4, 2026
The Teach-Back method is evidence-based and cost-effective. However, its implementation is inconsistent due to time constraints and lack of standardized training. Institutions must integrate literacy assessment into EHR workflows and allocate dedicated staff for medication counseling. Without structural change, educational interventions remain superficial.
Siri Elena March 4, 2026
Oh wow, a 38% failure rate? Shocking. 🤭 I guess the real issue is that people can't read. Or maybe they just don't care. I mean, if you can't figure out that 'metformin' is metformin, maybe you shouldn't be managing your own meds. Just sayin'. 😘
Divya Mallick March 5, 2026
This is what happens when you let Western medicine dominate global health narratives. In India, we've been using generics for decades. No panic. No confusion. Why? Because we don’t worship brand names like some kind of pharmaceutical cult. Your obsession with logos and colors is a symptom of capitalist delusion. Your system is broken-not your people.
Pankaj Gupta March 6, 2026
I appreciate the data presented here. The correlation between low health literacy and medication non-adherence is well-documented. However, the proposed solutions-visual aids, Teach-Back, pill apps-are only effective if they are accessible. We must consider digital literacy, cognitive load, and language barriers simultaneously. A one-size-fits-all approach will continue to fail marginalized populations.
Alex Brad March 7, 2026
Ask your pharmacist. Look at the label. Use the app. That's it. No fluff. No drama. Just do the three things. It's not hard.
Renee Jackson March 8, 2026
Every patient deserves clarity, not just those who can advocate for themselves. Healthcare systems must treat health literacy as a core competency-not an afterthought. Training for pharmacists, standardized visual tools, and multilingual resources aren't luxuries. They're ethical imperatives. We have the tools. We just need the will.
RacRac Rachel March 9, 2026
OMG I just learned this and I’m so emotional 😭 I used to be scared of my blue pills too! But now I scan them with Drugs.com and it’s like magic ✨ Same active ingredient? YES! I’m so proud of myself for asking questions now 💪❤️ #HealthLiteracyRevolution
Jane Ryan Ryder March 9, 2026
People stop taking meds because they’re dumb. Not because the system is broken. Stop making excuses. If you can’t read a label, don’t take pills. Let someone else do it. Simple.
Callum Duffy March 9, 2026
In the UK, we have a similar issue with branded vs generic statins. The NHS mandates generics unless clinically indicated otherwise. Patient education is embedded in the dispensing process. It’s not perfect, but it’s systematic. Cultural attitudes toward medication vary, but structure can overcome perception gaps.
Chris Beckman March 11, 2026
lol so like... the blue pill is the same? wow. who knew? maybe if people stopped being so lazy and actually read the label like 5 seconds they wouldn't be so confused. also why do we even have brand names if they're all the same? capitalism is dumb.
Levi Viloria March 12, 2026
In my work across rural clinics in Latin America and the U.S., I’ve seen the same pattern: when patients are shown side-by-side comparisons and given time to process, fear turns to trust. It’s not about intelligence. It’s about dignity. The real crisis isn’t ignorance-it’s being treated like a problem to be fixed instead of a person to be heard.